THE surgeon who operated on baby Augustine Somers while he was still in the womb described the life-transforming operation yesterday.
Professor Jan Deprest, a leading foetal surgeon, has carried out the landmark operation 45 times worldwide and has trained teams in Britain and around the globe.
The operation on babies diagnosed with spina bifida – when the spinal cord does not develop properly in the womb – gives them a better chance than similar surgery after birth because of the earlier intervention.
Professor Deprest explained how it involves opening the uterus and exposing the spina bifida without delivering the baby, repairing the baby’s spine before leaving it safely inside the womb.
There are risks but the potential benefits for infants can be life-transforming. In some cases it can lessen the damage before birth, allowing them to be able to walk and lowering the risk of brain damage.
Professor Deprest explained the intricate four-hour procedure does not repair any spinal damage already suffered by the unborn baby but will protect it from further harm.
From his home hospital in the Belgian city of Leuven, he told The Sunday Post: “We are not repairing any damage which may have happened already but stopping the clock on future damage to the open and exposed spinal cord in the womb.
“We work along with neurosurgeons who carry out the surgery on the baby’s spine.
“This is very much team-work.”
The surgeon stressed the astonishing procedure can only benefit some babies diagnosed with spina bifida in the womb.
American research, from the Children’s Hospital of Philadelphia, shows that of 2,404 mothers referred, only 341 were operated on, although doctors are optimistic that this figure will increase along with their skill and experience.
“Mothers whose babies have open spina bifida, where the spinal cord is exposed, can be considered for foetal surgery,” said Professor Deprest.
“It is the most common form.”
Professor Deprest is the director of the foetal surgery programme in Leuven, east of Brussels, where he is based at the University Hospital.
He also operates two days a week at University College Hospital in London.
He said: “We have a window of opportunity for surgery 24 to 26 weeks into pregnancy.
“The baby has to be viable should the mother go into early labour and not too advanced where damage to the spinal cord may be extensive. The baby risks being born early because surgery increases the likelihood of premature delivery.
“There is also a risk of the placenta haemorrhaging, which risks the mother and baby. This is around 5% according to a US study and that will always be the case.”
The procedure does not cure spina bifida but research shows it can reduce the severity of the disabilities usually associated with the condition.
The only British team carrying out the surgery is based at Great Ormond Street Hospital and University College Hospit, in London. The surgeons there were trained by Professor Deprest and, in October, revealed they had operated on two babies, the first in Britain.
Spinal surgery in the womb as an alternative to postnatal surgery means the defect is closed earlier, which prevents damage to the spinal cord in the last third of pregnancy.
Until now, mums could choose either to have the foetal surgery abroad, or in Britain after the baby is born. After the operations in London, lead neurosurgeon Dominic Thompson said: “In spina bifida, the spinal canal does not close completely, leaving the spinal cord exposed from an early stage in pregnancy.
“This results in changes to the brain, as well as severe trauma-related injuries to the nerves on the lower half of the body.
“Closure in the womb is an alternative to postnatal surgery, and improves short and medium-term outcomes.
“While neither intervention is fully curative, in foetal surgery the defect is closed earlier which prevents damage to the spinal cord in the last third of pregnancy.”
Professor Deprest said: “It is good to work with a team in the UK and collaborate in such valuable foetal surgery.”
He is now working on a keyhole version of the foetal surgery.
This would allow surgeons to operate using minimally invasive scopes and open less of the womb.
The technique is routinely used in other types of surgery, such as the removal of gall bladders. Professor Deprest has also carried out surgery on unborn babies to close their abdomens when they do not shut over, as is normal when the baby develops in the womb.
The condition is called diaphragmatic hernia.
Doctors have also operated to save the lives of twins when one takes all the nourishment from the placenta.
In the USA, an operation has also been carried out on an unborn baby to correct a heart defect before it went on to prevent the organ developing properly.
How the operation works
The pioneering in-womb surgery is steered by a theatre team of up to 30 multi-disciplinary specialists.
The mother is first given an anaesthetic, which passes to the baby.
The surgical team have to carefully monitor the vital signs of the baby throughout the procedure to ensure it does not become distressed.
Surgeons open the mother’s abdomen and uterus in a similar way to a caesarean section using an incision in the bikini line. The opening in the abdomen is slightly wider than the cut used for a caesarean, but is in the same place in the lower abdomen.
This is because it has to be big enough to allow the surgeons to safely lift the uterus, or womb, out of the mother.
Surgeons ensure the foetus is face down so they can expose the correct part of the baby’s spine to operate on.
This allows them to make an incision in the uterus and expose the spina bifida defect in the foetus. In the later stages of pregnancy the uterus is one of the most blood-heavy organs in the human body and surgeons have to take extreme care when cutting into it.
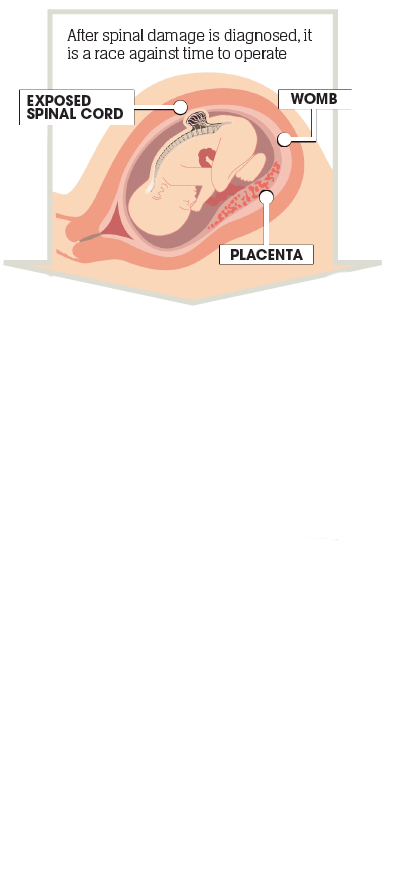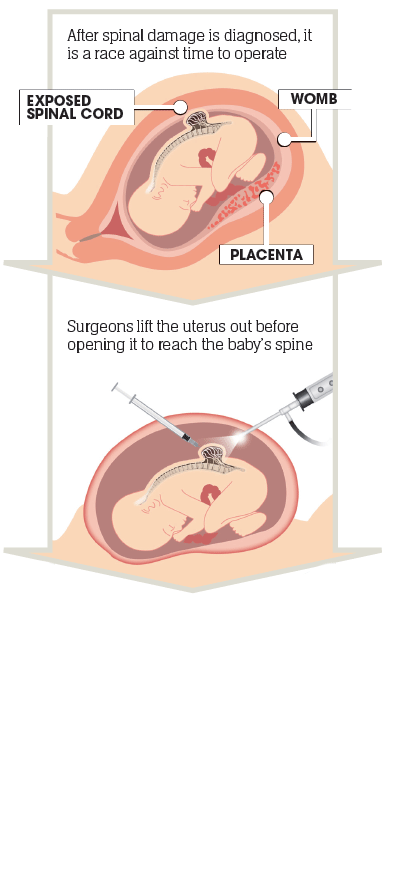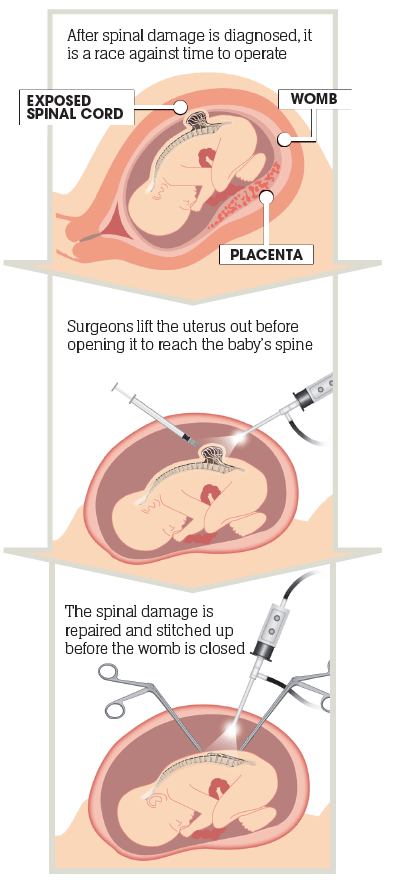
The neurosurgeon then cuts around the exposed spinal cord, which is protruding through a hole in the back of the foetus, to isolate the crucial nerve tissue. The spinal cord is separated from the surrounding skin and then put back into the spinal canal.
With the nerve endings protected inside the spinal canal, doctors have to close over the delicate membranes around the spinal cord which, on a tiny patient, is an incredibly complex task.
This allows them to create a new protective tube around the spinal cord.
The muscles and skin are then brought together and stitched closed. This protects the spinal cord and prevents leakage of further spinal fluid.
Finally, the uterus and abdomen are securely closed and the mother and baby are taken back to the recovery area.
The baby remains in the mother’s womb until approximately 37 weeks, before being born by caesarean section.
The procedure does not cure spina bifida but research shows it can reduce the severity of the disabilities often associated with the condition.
‘This will change the lives of babies and their families’ – Greg, 26, living with spina bifida
Greg Cumming believes open foetal surgery offers children with spina bifida the best start in life.
Greg welcomes surgical advances which can massively benefit children whose condition would otherwise have had a greater impact on their life.
He said: “It’s a positive thing that surgery can be done to give a baby the chance of improvements in their condition.
“You can’t get more positive than that.
“Having the benefits of the surgery before you are born will give them the best start to life.
“It has potential to transform the life of the baby and the lives of their family for the rest of their lives.”
The 26-year-old, who was born with the condition, said he found dealing with it hard when he was growing up and kept it secret for fear of being singled out.
The effects of spina bifida can include paralysis of the legs, incontinence and in severe cases brain damage.
However, the development of open fetal surgery means doctors have a new way to improve the lives of children with the condition – before they are even born.
The surgery can improve their ability to walk and reduce other health problems that result from the condition. Although Greg’s condition does not affect his legs it does cause urinary problems that mean he has to catheterise every day to stop his bladder from leaking.
As a result, he had to take a bag of pads with him whenever he went on school trips and feared other children finding out why he had his rucksack at all times.
Greg, from Grangemouth, accepts people’s experiences will differ but he explained that he didn‘t stop trying to hide his condition until he grew up.
“It’s a difficult condition to live with when you are younger,” he said.
“You try to hide away that part of your life. You try to hide it so people don’t pick on you.
“As I grew older I would think about what people would say. I thought no one would accept me.”
Greg, who organises a race night every year to raise cash for spina bifida charity SBH Scotland, is more susceptible to contracting urinary infections and last year had to seek treatment for 40 separate infections.
And while the condition has less of an impact on his life than some others living with spina bifida, it still makes some activities, like swimming, harder because of the added chore of catheterising and the risk of infection.

Enjoy the convenience of having The Sunday Post delivered as a digital ePaper straight to your smartphone, tablet or computer.
Subscribe for only £5.49 a month and enjoy all the benefits of the printed paper as a digital replica.
Subscribe

