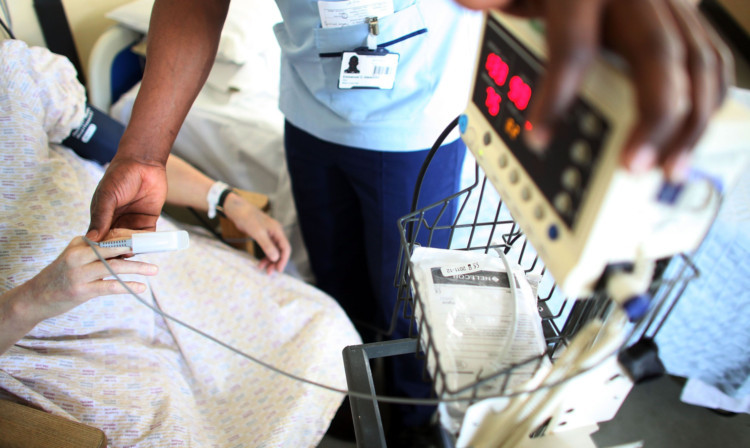
Claims that care services are ‘collapsing’ as the number of dementia victims being rushed to A&E wards has soared by 64% in just five years.
Furious critics claim the volume of sufferers being admitted to hospital shows England’s social care services are “collapsing”.
A shock Sunday Post probe has revealed as many as 600 emergency admissions or re-admissions are now made every day for dementia patients across England.
And the numbers of vulnerable patients being admitted is rising at a “worrying” rate with 219,064 admitted in 2011/12 compared to 133,373 in 2007/08.
Last night Labour’s shadow health minister Jamie Reed, who uncovered the figures, blasted: “David Cameron has cut council care budgets to the bone. Now the most vulnerable in society aren’t getting the care they need at home and their families are turning to A&E for support. These cuts to social care have added to David Cameron’s A&E crisis.
“Thousands of frightened and frail people are in the backs of ambulances the worst place for them to be. David Cameron needs to shore up England’s collapsing social care services. Our older people deserve much better.”
Campaigners are calling for new strategies for caring for people with dementia to try to reduce the nearly 900,000 patients who were admitted or brought back into hospital following earlier treatment, over five years.
Chris Quince, of the Alzheimer’s Society, said the “main factor” behind the increase in admissions is diagnosis rates which have gone up from a third in 2007, to 45% in 2012.
This means the number of people with dementia has risen from 700,000 to 800,000. But he claimed it has left hospitals struggling to cope.
He said: “However, this increase in emergency admissions of people with dementia demonstrates hospitals have to put good quality dementia care at the top of their priorities.
“The recent national audit of dementia care in general hospitals indicates many were struggling to deliver good quality care, with case notes showing assessments often not being conducted and many new and support staff not receiving training.
“It is vital, where possible, hospital admissions and re-admissions are avoided and to do this people with dementia need support and care in the community. Currently many people struggle to access care and support early enough.”
A Department of Health spokesperson said: “We want to improve care for people with dementia by improving diagnosis rates, and making sure people receive the right support in their community to reduce unnecessary A&E admissions. That’s why we made £3.8 billion available for better integration of health and social care.
“We have also set out proposals for the proper use of electronic health records and care plans with every vulnerable older person having a named GP accountable for making sure they receive this care.”
Vulnerable gran was sent home alone
A hospital in Cumbria apologised last week after it sent a grandmother with severe dementia home alone in a taxi wearing just a flimsy bed gown.
Medical staff even gave the driver the wrong address and his passenger Sylvia Dawson, 76, was incapable of telling him where she lived. When she eventually arrived at her home in Appleby, Cumbria, more than 30 miles away, she was said to be in a distressed state clutching a bag containing her clothes.
Mrs Dawson, who was diagnosed with dementia four years ago, was injured in a fall at home on Wednesday October 16. She was taken to Carlisle’s Cumberland Infirmary A&E depeartment. A few hours later her husband Terry, 80, received a call to say she could be sent home after a CT scan showed she had not suffered any serious injuries. She was put into a taxi and sent home with a male taxi driver to the wrong address. The man called Mr Dawson who guided him to the correct place.
Several days after the harrowing incident Mrs Dawson’s condition deteriorated and she was transferred to a nursing home.
North Cumbria University Hospitals NHS Foundation Trust which runs the hospital apologised and launched an investigation.

Enjoy the convenience of having The Sunday Post delivered as a digital ePaper straight to your smartphone, tablet or computer.
Subscribe for only £5.49 a month and enjoy all the benefits of the printed paper as a digital replica.
Subscribe